


Staffing issues have caused pressures in Health with waiting lists increasing across several services, including adult mental health, while the lack of capacity in local care homes has led to unnecessarily longer stays in hospital, according to a new report.
Health's Quality and Performance review for December 2021, the second of its kind, shows that the department failed to meet 50% of expected standards.
The first iteration of the report, which covered the year to June 2021, was released in August 2021 after initially being withheld from the public over concerns about "sensationalised" media reporting.
The 'Quality and Performance Report' covers the entire health estate, not just Jersey's General Hospital. It sets a number of 'best practice' standards, and ranks performance using a traffic light system - either green, amber or red.
CLICK TO ENLARGE: A table showing demand and activity across health departments.
At the end of December 2021, 23 areas were in green, three in orange and 26 in red.
Express breaks down the report's key findings, and shares Health officials' explanations for each...

Pictured: The average waiting time in A&E peaked at 182 in December.
Over 2021, the average waiting time in the Emergency Department (ED) was 163 minutes - but that figure was exceeded over seven months, with December hitting a maximum of 182, despite a smaller number of patients attending that month.
This area was, however, on target, as is the average length of stay for emergency inpatients, which has remained green throughout the year with 5.7 days.
The department attributed the increase in December to a higher number of covid-19 admissions which required “additional logistical arrangements”, as well as patients who had a “prolonged” stay in the department due to requiring “safe discharge” at home to prevent unnecessary admission to the hospital.
Several of the problems identified in the previous report however remained present in the second half of the year.
Patients not being 'triaged' within 15 minutes of arrival: in 2021, a third of patients had to wait longer than 15 minutes to be dealt with. Since June, the proportion of patients seen during this period has dropped slightly and even reached a year low in September with only 60.1%.The department said simultaneous arrivals result in “difficulties” in this area within the current workforce model for the Emergency Department.
Patients left waiting in A&E for more than 10 hours: 180 patients were left waiting more than 10 hours in the Emergency Department in 2021, with the rate continuing to go up since June. In December, there were 29 patients in that situation.
Discharges before midday: The number of patients discharged at midday has also continued to drop since July 2021, reaching just 13% in December.
Emergency patients returning within 30 days: The rate of emergency inpatient readmission within 30 days of discharge was consistently in the red throughout 2021, with numbers having slightly increased since June 2021. Overall, 12.5% of patients cane back within that 30 day timeframe in 2021.
The report says that the Emergency Department and Site Management services are “developing options and reviewing escalation processes” to see what can be done to improve performance in these areas.
Meanwhile, the proportion of patients receiving treatment within an hour of their arrival at the Emergency Department has gone in the red, dropping from 71.5% in June to 63% in December 2021.
This was said to be due to an increase in short-term sickness according to the department. Whilst temporary cover was found, it was not available for all shifts.
Average ambulance response times for 999 calls were not provided in this latest report.
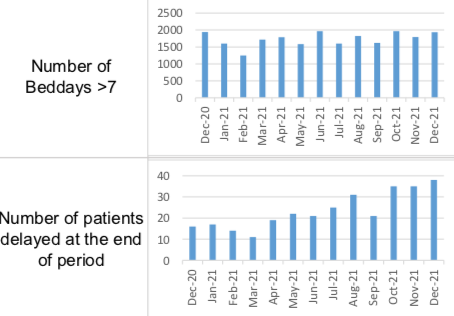
Pictured: The length of stays and the number of delays at the end of a stay were both increasing in the later part of the year.
Issues within the local care sector have driven up both the length of stays and the number of delays at the end of a stay.
The number of patients who stayed for more than seven days in hospital reached 1,937 in December. This marker was in the red and amber five times in the last six months of 2021.
Meanwhile, the number of patients delayed jumped from 21 in June to 38 in December.
“This was due to a lack of capacity within the domiciliary home care market and care home market,” the department said. “A discharge support team has been implemented to support patients with short term care at home whilst awaiting capacity with a mainstream provider.”

Pictured: The health department is currently doing work to understand why the number of c-sections has increased.
The number of elective and emergency C-section rates remained high throughout 2021, with more than one birth in three, topping 46.5% in November 2021.
The Department said a review of C-sections had revealed that a large proportion of women (67%) who had not had a baby before were induced, resulting in emergency C-sections. “A deep dive is underway to understand the factors contributing to this increase,” they added.
In addition, nine women who gave birth in December, where the combined C-section rate was 40%, had had a previous C-section. Of those, eight (89%) resulted in a repeat section.
The department said there is a VBAC (Vaginal birth after caesarean) clinic is in place to counsel women, whilst further review is underway to look into ways to reduce repeat C-sections.
Meanwhile, the number of home births has fluctuated throughout the year but mainly remained in the amber and green areas, with the average for the year, 4.5%, just below the standard of 5%.
CLICK TO ENLARGE: The figures for the maternity department.
Through the last quarter of 2021, the length of stay on the maternity ward remained below the standard of 2.3 days.
Whilst the department says there has been “improvement” in the percentage of women experiencing postpartum haemorrhage, it remains in excess of the desired standard of 2.9% with an average over 2021 of 7.8%.
“The improvement programme is progressing and being managed through the intra-partum care group,” the report notes.
The department also said a risk assessment tool is being trialled, which includes the use of Syntometrine – an injection that causes contraction of the muscles of the womb - as opposed to relying on oxytocin alone, in cases where women are deemed to be more at risk of haemorrhaging.
The number of women having induced labour also exceeded standards throughout the whole year, with almost one in three births (27.4%). A Labour Ward Forum has started work this month and will focus on induction of labour in order to achieve the desired 25% cap.
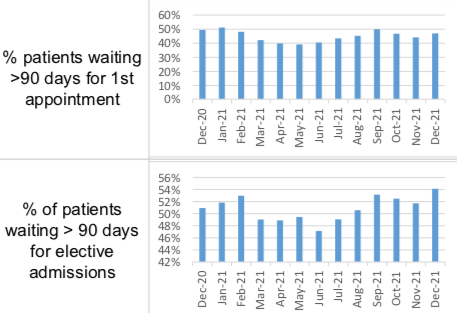
Pictured: The number of patients waiting for their first appointment and their elective admissions remained for more than 90 days remained high in 2021.
Figures show that 84% of patients awaiting community dental and orthodontic services and 35% of patients awaiting acute services are waiting for more than 90 days.
The numbers of outpatients waiting for their first appointment, and of inpatients awaiting elective treatment for more than 90 days both remained in the red for the year with an average of 47% and 54.1% respectively.
The department said the increase in the number of patients awaiting inpatient treatment over the last quarter of 2021 was linked to an increase in the “relative number of additions to the waiting list associated with the increased outpatient activity”.
“Compared to pre-pandemic levels there has been an overall growth in the volume patients waiting of 14%,” they said. “The elective waiting list at end 2021 is 10% lower than at the end of 2019 (pre-pandemic).”
“When compared to pre-pandemic levels, the total number of people waiting for a first outpatient appointment is minimally higher (0.8%),” they added.
As of 31 December 2021, there were 3,353 patients who had been waiting for more than 90 days without an appointment date.
The department noted that there has been an “evident” reduction in the number of patients awaiting acute secondary services when compared to pre-pandemic levels, with the total number of patients awaiting their first appointment reducing by 13%.
“Analysis of referral and activity data has shown that the reduction in the acute secondary care waiting list is driven by increased activity during 2021 as opposed to a reduction in referrals,” they said.
Whilst the number of patients who did not attend their appointment rated green from January to June 2021, it was in red from five out of the remaining six months of the year. After jumping from 7.3% to 8.7% between June and July, the numbers dropped in August with 7.6% and then consistently increased over the following four months, reaching 9.2% in December.
Pictured: The waiting list for dental services has seen a 122% increase.
Meanwhile, analysis of the community waiting list showed a 122% increase in the number of patients awaiting treatment from dental services.
In July 2021, Health and Community Services launched an appeal for volunteers as part of its’ ‘Oral Health Strategy’ which aims to improve the quality of services by reducing waiting lists and inequalities in the access to dental care, as well as reducing the number of people suffering dental decay and oral cancer.
Meanwhile, Sarah Pollard, the co-founder of Super Smiles, a local dental charity, said in November that children were waiting seven years for Orthodontic treatment with over 5,000 children are awaiting a dental appointment in the community department.
The department said the waiting times are being addressed through a Task and Finish programme which includes measures to increase capacity but also manage demand appropriately.
Challenges continue within elective services, in particular Trauma and Orthopaedics, Ophthalmology and General Surgery.
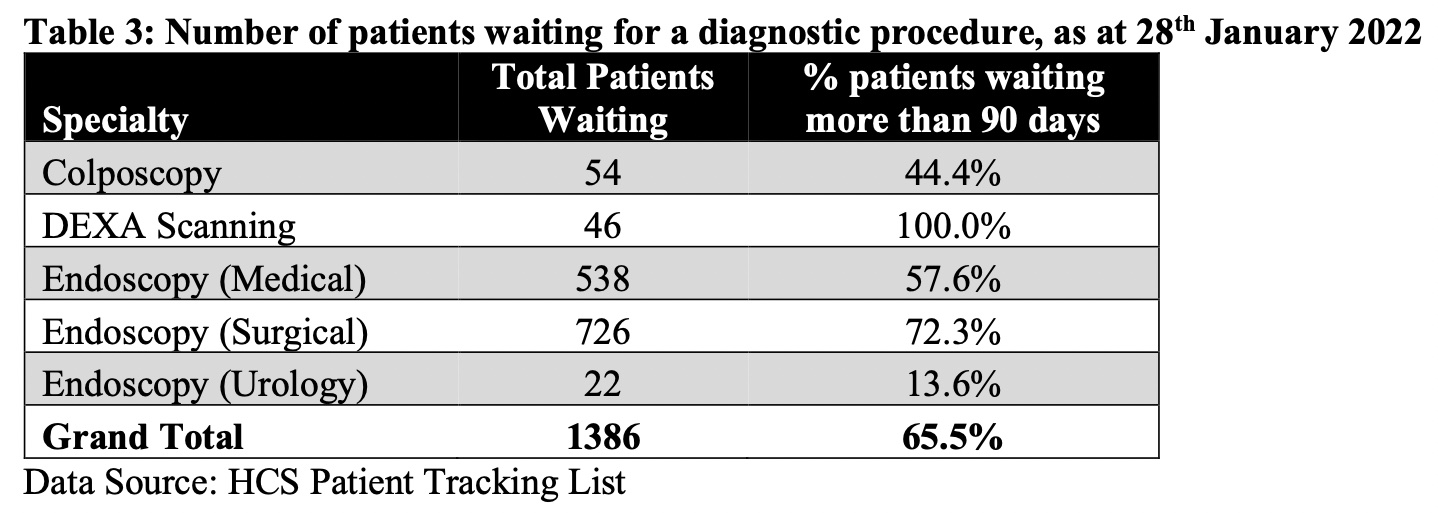
Pictured: Waiting list figures provided by the Health Minister.
Between the end of 2019 and end of 2021, the number of patients awaiting a procedure went up 74%.
Endoscopy involves looking at organs inside the body with a thin and flexible tube with a light and camera called an endoscope. Images of the inside of the body are then surveyed by medics on a screen, helping them to understand the potential source of unusual symptoms and screen for cancer and other conditions.
“This growth is linked to a reduction in the volume of activity during the immediate COVID response and subsequently, reduced throughput due to enhanced IPAC requirements,” they wrote.
Figures published by the Health Minister in January 2022 showed there were 1,386 people waiting for a diagnostic procedure – with around three in five of them having to wait more than 90 days to be seen and the bulk of the backlog – 1,286 - relating to endoscopy procedures.
“The rate of growth has slowed in the second half of 2021,” the Health department noted in the report. “It is anticipated that the introduction of the FIT (Faecal Immunochemical Testing) programme and reviewing capacity by the clinical team will enable recovery to pre-pandemic levels within 2022.”
Meanwhile, there was a 25% reduction in the number of under-18’s on the elective waiting list in 2021 and hospital stay lengths continued to rate green throughout the second half of the year.
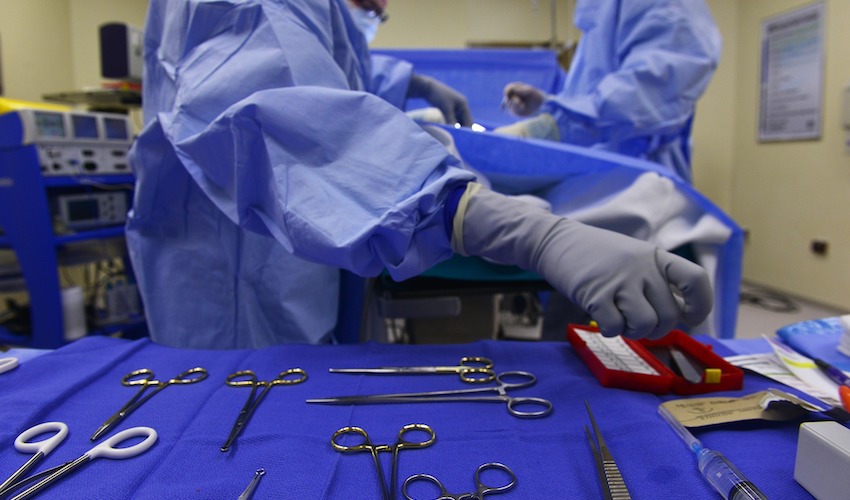
Pictured: Hospital theatres are still not being used as well as they should be.
Officials highlighted the underuse of the hospital's theatres as one of the “top three" improvement priorities in June 2021.
At the time, Director General Caroline Landon said this was because surgery scheduling processes were not good enough.
She said the department was looking at introducing a 'Theatre Direct Service' where patients don’t have to sit on the wards unnecessarily and then come into the theatre, whilst a 'Task and Finish Group' had been set up to address the issue.
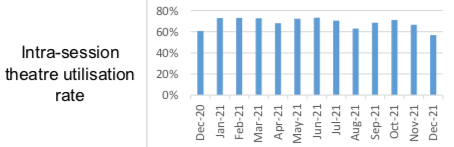
Pictured: The theatre utilisation rate was down in December 2021.
In October, Express revealed that non-urgent procedures had had to be rescheduled due to staff shortages, and medics were put on alert that private operations may have to be suspended if problems continued.
Since then, the ‘utilisation rate’ has reduced, reaching just 56.7% in December 2021, which the department attributed to “reduced activity” due to staffing and inpatient constraints.
They also said there were data quality issues with the metric as it does not currently include day surgery and minor ops activity.
Mental health services continued to experience a high level of demand across a range of services in the second half of last year.
The number of referrals for Adult Mental Health services and Jersey Talking Therapies increased by 6% and 23% respectively between 2020 and 2021.
Bed occupancy rates increased over the second half of the year, exceeding standards in August, September and November.
In the introduction to the report, the department acknowledged that occupancy in the older people’s inpatient service remained high. They said there was an increasing number of service users who are in hospital despite not needing to, because they no clear discharge pathways as a result of lack of appropriate available community provision.
“This is being jointly reviewed by the service and social care,” they said.
Over the period, there was one young person under the age of 18 admitted which the department said was “clinically appropriate in the absence of any available alternative specialist bed”. Meanwhile, there were five adults admitted in the acute services, three less than in the first half of 2021.
The figures show that at the end of December, there were 278 islanders waiting for their first assessment with Jersey Talking Therapies (JTT) or the Psychological Assessment and Therapy Service. 106 of those had been waiting for more than 90 days.
Meanwhile the number of JTT clients waiting to start their treatment continuously dropped since the end of June, reaching 212 in December.
The number of those who have been on the waiting list for over 18 weeks, also dropped between July and November, when it reached 74 but then picked up again to 102 in December.
The department said this was due to “high levels of demand, reduced staff capacity (due in part to vacancies, sickness and leave) and a backlog associated with the initial period of covid-19”.
“The mental health services are currently developing a recovery plan to address this,” they said.
“Mental health services are also currently reviewing their Quality and Performance metrics as part of the wider service development plan.
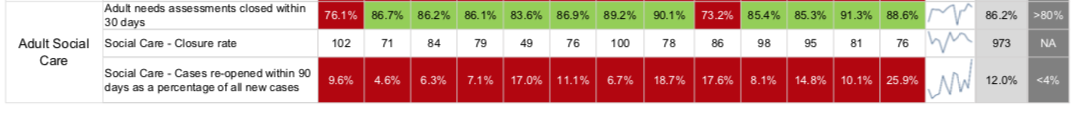
Pictured: The number of assessments closed within a month slightly dropped from 90.1% to 88.6% between June and December 2021.
Issues have also arisen in adult social care with a “significant” increase in the number of cases reopened within 90 days, which jumped from 6.7% in June 2021 to 25.9% in December 2021.
“This sudden and significant increase in cases reopened is being examined in detail by the service in order to properly understand this and identify the contributory factors, in order to address this,” the department said.
Meanwhile the number of assessments closed within a month has slightly dropped from 90.1% to 88.6%, which remains higher than the standard of 80%.
The report lists key figures relating to patient safety and infection control in the year to date:
Patient safety incidents: 2,029 reported between July and December 2021, making a total of 4,063 in 2021.
Falls resulting in harm: Numbers reduced in the second half of 2021 from 61 to 46.
Pressure ulcers acquired as an inpatient: 97 over the year, the majority of which, 54, came in the last six months of the year. There was a peak of 14 in December, which the department attributed to staff being encouraged to submit information about incidents via the Tissue Viability Nurse. Further educational events are being planned this year to raise awareness of pressure ulcer care and improve documentation.
More serious pressure ulcers acquired as an inpatient: There were six between January and May 2021 but none after that.
MRSA: 0.
C-Diff: 6.
Despite Chief Nurse Rose Naylor previously describing rates as “not acceptable”, the process of responding to complaints within 28 days has remained in the red between July and October (figures were not provided for November and December 2021 as they are reported two months in arrears).
On average, just over 58% of the 130 complaints received an answer within a month during that period.
A total of 140 compliments and 59 comments were sent during that time.
The department said there is “continued improvement” in responding to complaints in a timely manner.
They said a number of actions have been taken recently whose impact has not yet been assessed, this includes training for customer care and communication skills and the creation of a Patient Advice & Liaison Service (PALS) desk at the hospital outpatient department to deal with queries and resolve low-level issues.
Standards were achieved in several areas in December, however, after failing in June 2021:
Other areas where standards were achieved at the end of December included:
Comments
Comments on this story express the views of the commentator only, not Bailiwick Publishing. We are unable to guarantee the accuracy of any of those comments.