


Over-reliance on Ivan Muscat, the need for a Nightingale staffing plan and better record keeping were among the key lessons to be learnt from the first official review of the health response to the pandemic, which concluded that the Government was overall successful at pursuing a strategy of “least overall harm."
Published this morning by Comptroller and Auditor General (C&AG) Lynn Pamment, the report was the second in a series analysing how the pandemic was handled.
Last month, she concluded that emergency scheme launched to support those who lost their job due to the pandemic and who had been in the island for fewer than five years was “necessary”, but that there were overpayment issues, leaving Government officials still trying to recover more than £75,000.
In her latest report on the healthcare response, she identified positive aspects in the response as well as areas for improvement and made a series of recommendations, including a ‘lessons learned’ exercise to be undertaken across the whole health and care system.

Pictured: The Comptroller and Auditor General (C&AG), Lynn Pamment, has been reviewing the Government’s response to the covid-19 pandemic.
“Jersey has not experienced the significant rates of covid-19 infections that other countries have,” she wrote.
“As at 31 December 2020 the total of number of confirmed covid-19 cases in Jersey was 2,760 and the total number of covid-19 deaths was 44, which represents 1.6% of all confirmed cases. The public health advice given has been effective when assessed against a strategy of least overall harm.”
Early action
The Government started taking action "early in 2020 to start to understand and monitor covid-19 and its potential impact on Jersey", and "Senior Health and Community Services staff were aware of the key risks from covid-19 from an early stage."
No gaps in hospital staffing
Ms Pamment noted that, despite high level of healthcare staff absences in March and April 2020, the hospital and community system did not experience any “significant gaps” during the first wave thanks to low numbers of covid-19 patients, and the suspension of non-urgent procedures, which freed up staff.
However, this has contributed to waiting lists growing. For example, the number of patients waiting for an outpatient appointment has gone from just above 8,000 in January 2019 to over 10,000 by the end of November 2020. As at 26 February 2021, it stood at 9,289.

Pictured: Cancelling non urgent procedures helped prevent staff shortages during the pandemic.
Community cohesion
Ms Pamment also highlighted the Community Bronze Group – in which independent organisations, such as nursing and residential care homes, reported on risks and issues - as an area of “good practice”, as they prompted HSC to move staff to help with shortages.
GP partnership
The Government’s contract to employ GPs to ensure the continuity of services was also said to have resulted in “benefits to patients”.
Care plans
In addition, Ms Pamment highlighted the community care plans put in place for vulnerable patient groups in the community, such as the elderly.
These plans sought to ensure continuity of services during the period when a different model of primary and community care operated due to the pandemic.
Relying on a 'key man'
One of the key takeaways was the need to expand public health, as much reliance had been placed on Dr Ivan Muscat.
Ms Pamment suggested reviewing the public health function proposed as part of the Jersey Care Model to ensure it is “properly equipped to address future health protection emergencies."
She noted in her report that at the beginning of February 2020, it had been operating at “limited capacity”. Due to the planned sickness absence of the Medical Officer of Health, Dr Susan Turnbull, Dr Ivan Muscat was appointed as one of two Deputy Medical Officers of Health.

Pictured: The C&AG described Dr Muscat's “specific combination of experiences” as vital to the challenges caused by the pandemic.
Ms Pamment said Dr Muscat’s workload was “considerable”, adding that his “specific combination of experiences” - he is a microbiologist and a consultant in communicable disease control - had been “relevant and vital” to the challenges caused by covid-19 and helped the technical implementation of on-island testing, as well as advice on the wider pandemic from a population perspective.
However, Ms Pamment said the ‘key man’ risk of having a single point of expertise had materialised in the early stages of the pandemic when Dr Muscat was not available to provide updates on infection control.
Record keeping
The C&AG noted there was a “limited audit trail” regarding the advice received by the Government before and after Scientific and Technical Advisory Cell (STAC) was established. “This lack of record keeping means there is very little evidence of why specific public health advice was given, as opposed to alternative advice,” she wrote.
There was no record, for example, of why Jersey had not included Vietnam, Cambodia, Laos and Myanmar on its compulsory 14-day quarantine list in February, in contrast to the UK. Decisions on which face-to-face health services would be suspended and which would not were also not "supported by consistent documentation against a clear set of risk-based criteria."
While things improved after STAC was created, Ms Pamment said the record of final advice given had not been comprehensive, while there were no detailed records of the discussions around how the advice had been created. In addition, there was no “open and transparent” record of the sources STAC had relied to provide their advice.

Pictured: Ms Pamment said the minutes of the STAC meetings lacked detail in some areas.
“The minutes of the STAC meetings do not always include details of the advice STAC uses, the advice it rejects and the advice it amends and why,” the C&AG wrote. “In addition, the minutes do not contain useful action plans or an audit trail of follow through of actions taken."
Role of STAC
Ms Pamment also highlighted how the role of STAC had not been consistent during the pandemic – while the cell was heavily involved in advising the Government on how to reopen the island as well as border controls, they were not consulted regarding restrictions over the Christmas period, which eventually led to last-minute changes.
She recommended the creation of a Code of Practice for future STACs that would include "principles and procedures to be followed in determining membership, relationship with the sponsor department within Government, independence and objectivity, working practices and communication and transparency."
Nightingale Wing
The report also mentions that the decision to build the Nightingale Wing in April 2020 was driven by concerns that there could be a 248 hospital bed 'gap' based on a 'worst case scenario' model by Public Health England.
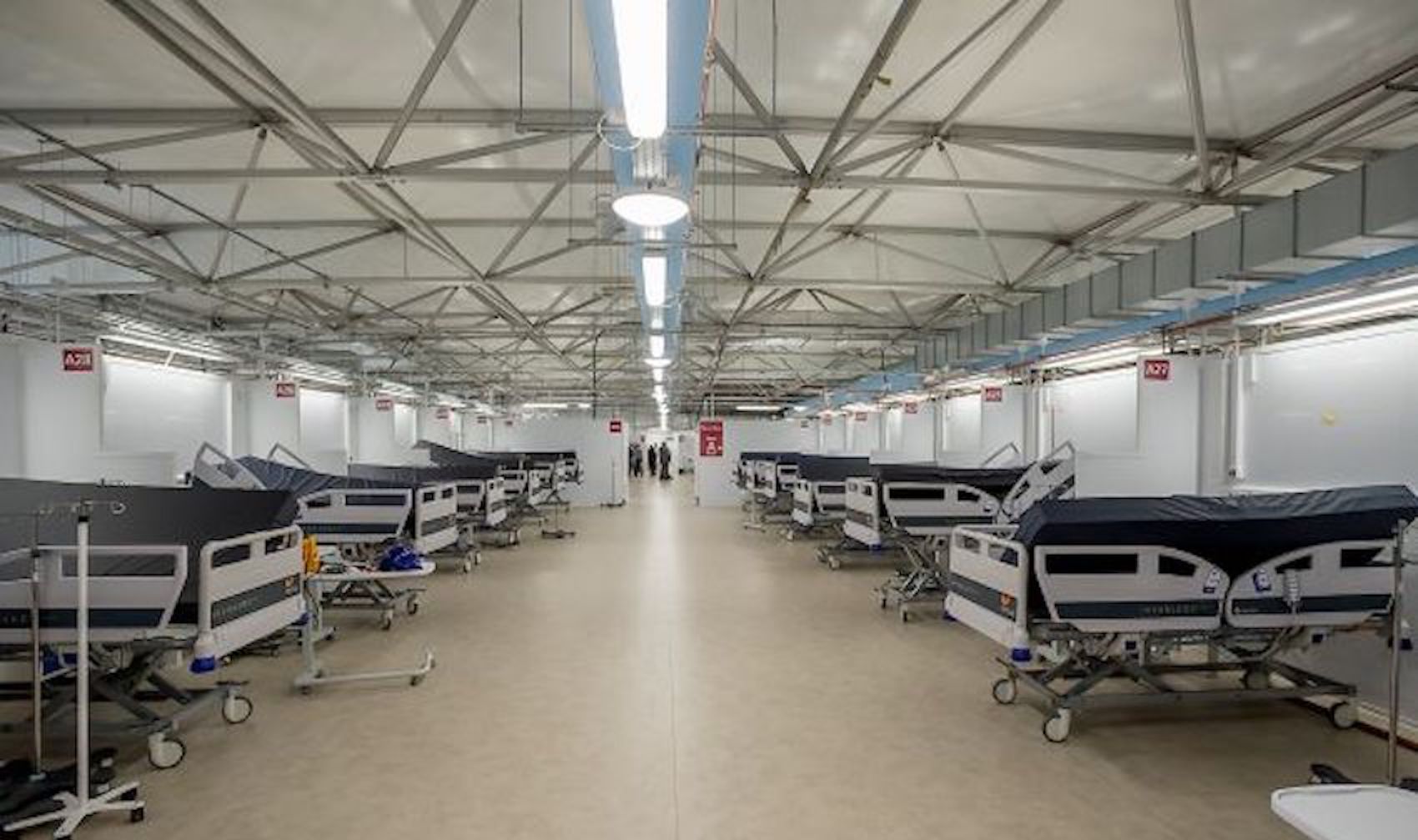
Pictured: The C&AG said there was no clear plan on how the Nightingale would be staffed.
Ms Pamment said it was not clear where the staff required to support the temporary facility's 180 beds would be found.
She also said the business case to extend the period of operation of the wing only included a “limited risk assessment."
PPE
While staff training needs were “appropriately identified” during the pandemic, mask training was rolled out “inconsistently”, particularly in March 2020.
“There was poor formal documentation of who had received training, variable compliance with the requirement to undertake training, a lack of equipment to test with, changing PPE guidance and a loss of a laptop containing evidence of who had passed and failed the training,” Ms Pamment wrote.
"Also during the second half of March 2020, a decision was made to transfer a number of patients from Samares ward at Overdale to the Sandybrook nursing home at St Peter. The patients transferred were not screened for covid-19 and staff at Sandybrook were not advised to wear Personal Protective Equipment (PPE), although PPE was available to all staff. Subsequently, staff from Sandybrook had to self-isolate," the C&AG noted.
Occupational health
Meanwhile, concerns were raised about the quality of the Occupational Health service.
The C&AG said some described it as being more focused on “getting staff back to work” than on a more “proactive offer that supports staff health and wellbeing in a more rounded way”.
The C&AG has made a number of key recommendations to the Government she believes should be prioritised in the wake of the review.
These include:
Review expansion of public health to make sure it is well-equipped to address public health emergencies in future
With any new public health advice, conduct assessments to take into account impact on vulnerable communities
Undertake a formal reflective evaluation of all the lessons learnt about business continuity planning in 2020
Review covid-19 experience to draw up a plan for dealing with future infectious diseases and produce a full public report
Work on reducing waiting lists and the cancer screening backlog
Review Occupational Health service and ensure services in future include access to counselling and support
Undertake a 'lessons learnt' exercise to understand staff's physical and emotional wellbeing needs and build these into future training programmes
Comments
Comments on this story express the views of the commentator only, not Bailiwick Publishing. We are unable to guarantee the accuracy of any of those comments.