


Lengthy waiting times for outpatients and inpatients, mental health services, and underused theatres are among the key problems facing the health service, according to a Government report initially withheld from the public.
Health's Quality and Performance review for June 2021 shows that nearly 20 key areas need improvements.
It was released yesterday, alongside an apology from Senior Officials for previously commenting that they did not wish to release it over concerns about "sensationalised" media reporting.
Health and Community Services Director General Caroline Landon said that her department is now making an effort to be "much more transparent around what we do, and recognising that we are public servants and that this data actually belongs to our patients, not to us."
The 'Quality and Performance Report' covers the entire health estate, not just Jersey General Hospital. It sets a number of standards, and ranks performance against each as either green, amber or red.
Of these, 17 categories were green (meaning they have met standards), three were amber and 16 were red.
Express breaks down the report's key findings, and health officials' explanations for each...
Several problems with the emergency department’s processes were flagged between June 2020 and June 2021, including:
patients not being 'triaged' within 15 minutes of arrival: over 2021, around one-in-four patients on average had to wait longer than 15 minutes to be dealt with. This criteria remained 'red' for the entire year.
Patients left waiting in A&E for more than 10 hours: 108 patients were left waiting more than 10 hours in the Emergency Department, and the rate has been going up over the last four months.
Discharges before midday: Only 14% of inpatients were discharged before midday, resulting in longer waiting times in the Emergency Department for patients needing a bed. This was 11% under the benchmark target of 25%.
Emergency patients returning within 30 days: The rate of emergency inpatient readmission within 30 days of discharge was consistently in the red throughout the year, with 12.6% of patients coming back within that 30 day timeframe.
The report said a ‘Patient Flow Working Group’ has been established to review the systems in place to address the issues with Emergency Department triaging.

Pictured: 108 patients were left waiting more than 10 hours in the Emergency Department.
On the rate of emergency readmissions, Group Director Rob Sainsbury explained that Health thought there might be a data quality issue and that “some of this data might be picking up patients coming back into hospital for more planned care.”
On the other hand, the average length of stay at the Emergency Department between in 2021 sat at 157 minutes.
This was on target, as was the average length of stay for emergency inpatients, at 5.8 days.
Average ambulance response times for 999 calls were not graded red, green or amber. The data showed that these varied across the year, with an average response time for the most critical cases standing at 6m52s, and 8m57s for other cases.
More than a third of deliveries across the time period - both planned and unscheduled - were C-sections. This was 12.5% over Health's benchmark ‘green’ target.
This was something Head of Midwifery Dana Scott said she wanted the Department to bring down, though she also noted that they wanted “to keep in mind women’s choice.”

Pictured: The report said the number of C-sections were not in line with standards.
One of the other ‘red’ alerts related to the number of postpartum haemorrhages - blood loss after birth.
8.4% of patients experienced it in the year to date.
This was linked to the number of induced labours - one in four women - which were also in the ‘red’ category. They were 2% higher than the benchmark standard.
CLICK TO ENLARGE: A breakdown of figures for the maternity ward.
The Department said it had set a number of key targets to tackle these issues and are "increasing [their] public health messaging to inform people of the benefits and risks of elective C-sections."
Last week, it was also announced that the ward would be getting a £6.5m refurbishment, which should be complete by October 2023.
In the meantime, women experiencing normal pregnancies are being recommended home births. 25 have taken place this year so far, compared to just eight in 2020 and 20 in both 2018 and 2019.
As of June, two-in-five outpatients were waiting more than 90 days for their first appointment, while nearly half (47.2%) of inpatients awaiting elective treatment were also waiting over 90 days.
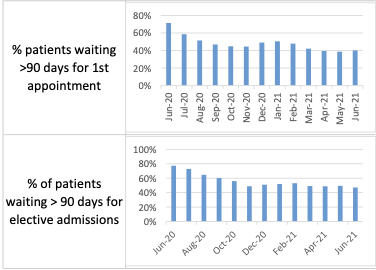
Pictured: Nearly half of inpatients are waiting over 90 days for their elective appointments.
Mr Sainsbury said that the pandemic had impacted on waiting times, with measures such as social distancing in the hospital reducing the number of patients they could hold, particularly during the first and second waves.
To tackle the issue, he said that Health had established a “a patient tracking list… so that we prioritise patients according to need and length of time they wait.”
The report showed that the hospital had seen a a reduction in ‘Do Not Attend’ rates - the number of people missing appointments.
Hospital stay lengths were also consistently rated green.
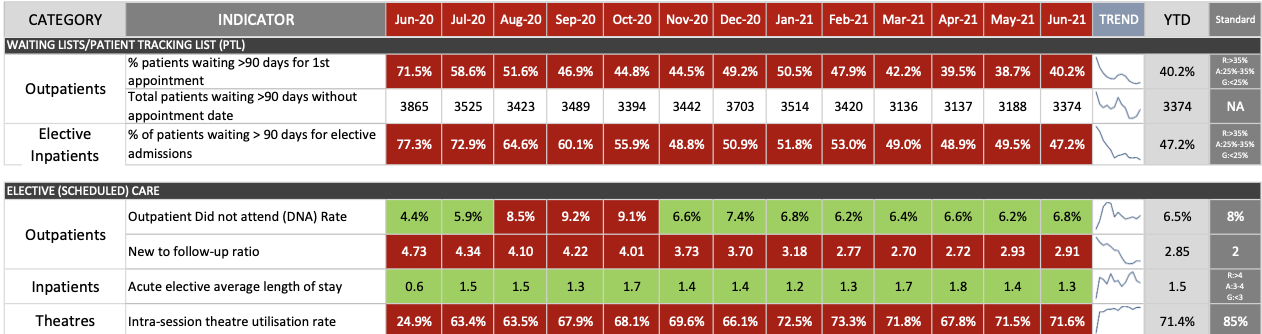
Pictured: Community Dental, Ophthalmology, General Surgery, Endoscopy, and Trauma and Orthopaedics were among the departments most hit with capacity issues.
Endoscopy, Ophthalmology, General Surgery and Trauma and Orthopaedics, meanwhile, are all struggling to keep on top of waiting times.
But Health said 'recovery plans' are in progress for both Endoscopy and Ophthalmology with capacity scheduled to increase in the third quarter of the year.
In respect of outpatients, waiting time issues are predominantly affecting Community Dental Service, Ophthalmology and General Surgery.
Work is underway with the Dental and Ophthalmology services to create additional capacity, and a similar programme being established for the General Surgery, officials said.
One of the “top three" improvement priorities is the underuse of the hospital's theatres, officials said.
It remained 'red' throughout the year, with 28.6% of available theatre space going unused on average.
Pictured: Dealing with the underuse of theatre space is a "top three" priority for the Health Department.
Director General Caroline Landon said this was because surgery scheduling processes were not good enough. She said more had to be done to ensure patients had pre-op assessments in a "timely manner" and that all the right equipment is in place in theatres "so we can ensure we are maximising our precious theatre time.”
She explained that they are now looking at introducing a 'Theatre Direct Service' where patients don’t have to sit on the wards unnecessarily and then come into the theatre, and a 'Task and Finish Group' has been set up to address the issue.
Following previous reports from Express on children being admitted to acute adult facilities for mental health issues, this new report confirms that seven children were put in Orchard House between June 2020 and June 2021, with four being admitted this June alone.

Pictured: Seven children were placed in adult mental health facility Orchard House.
Whilst bed occupancy levels mostly met standards across the year, there were some months that veered into the red.
In particular, since November 2020, acute admissions per 100,000 population have been consistently rising for older patients admitted to Beech/Cedar House, with admissions now hitting the red at 46.3 in June, 8.3 above the green target standard.
Across six months of Older Acute Care at Beech/Cedar House, the length of stay was marked as 'red'.
The report states that these Older admissions are “noted to be higher than National Benchmarking standards per 100K population”, and that a review has been undertaken to investigate them, as well as a recruitment drive for vacant posts.
The number of patients missing appointments has remained low, with levels marked as green throughout the year.
Adult Needs Assessments closed within 30 days have also improved across the year, starting in the red in June 2020 at 79.1%, but rising to and staying consistently green from January this year, sitting at 89.2% by June.
The number of clients waiting over 18 weeks for their Jersey Talking Therapies treatment to begin remained in the ‘red’ throughout the year, with two in five clients falling into that category.
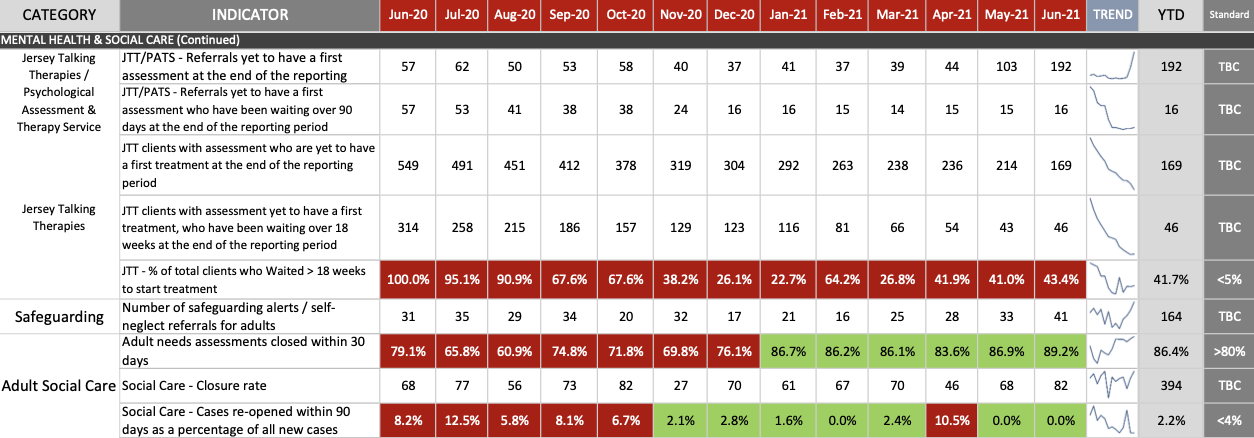
CICK TO ENLARGE: Two in five clients of Jersey Talking Therapies waited more than 18 weeks for their treatment to begin.
This is significantly higher than the target of below 5%, and a plan to “backfill posts, ongoing caseload monitoring and allocation”, review the pathway to treatment is ongoing.
The report listed key figures relating to patient safety and infection control in the year to date:
No benchmarks have been set for what would constitute red, green or amber in each of these categories.
Asked why by Express, Ms Landon explained Health was waiting for a new Director of Quality and Safety to be appointed first.
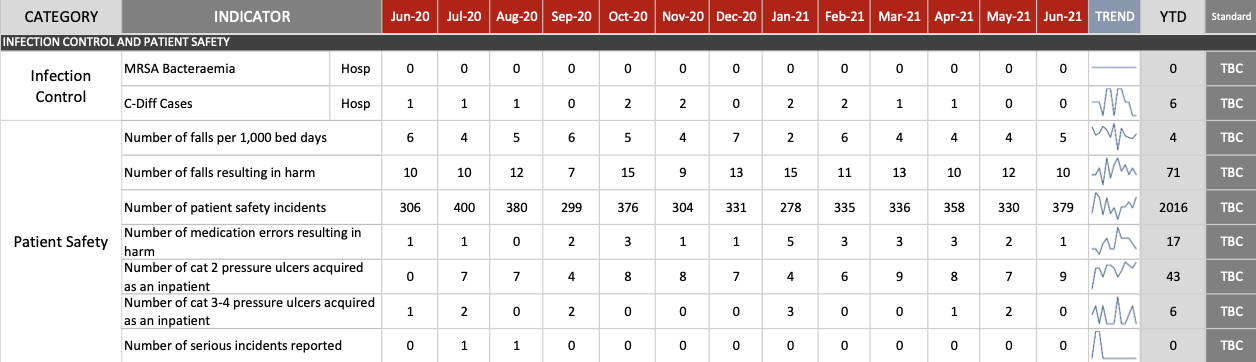
Pictured: There are no quality indicators for the infection control and patient safety figures, with department waiting on a Director of Quality and Safety to be appointed.
“You would quite rightly be expecting us as a health provider to be producing a quality account, and we don’t,” she said.
“This will be one of the first priorities for the Director of Quality and Safety when they are appointed - my aspiration is that as an organisation, we produce a quality account next year, and within that quality account will be all our pre-determined metrics.”
Turning to the patient safety incidents, Chief Nurse Rose Naylor and the Health team explained that higher numbers were seen as a good thing, as they suggested an open culture of learning from mistakes and "near misses". Health said they would like to see this number rise further.
An area which Ms Naylor told Express was “not acceptable”, however, was the continued red and amber ratings for the process of responding to complaints within 28 days.
In total, 28% of complaints were not responded to within 28 days in 2021, 59 in total.
“It’s not acceptable - these are people that are already not happy about the experience they’ve had with our service and to take an extraordinary length of time to respond to their concerns isn’t something we are proud of or think is appropriately,” Ms Naylor said.
She explained during the briefing that “we have got a benchmark in relation to this and… we have struggled to meet it."
She continued: “It’s an area of significant focus for us, and we’re working really hard with the care groups to support them in terms of how they respond to complainants.
“We’ve seen significant improvement particularly across some of our care groups in relation to something called local resolution - this is really encouraging people to have early conversations once complaints come in to see if we can solve the complaint in real time."
While several areas were highlighted for improvement, the report also celebrated several standards that had been achieved:
Follow Express for further analysis of the report and its findings in the coming weeks...
CLICK TO READ: The full report...
Comments
Comments on this story express the views of the commentator only, not Bailiwick Publishing. We are unable to guarantee the accuracy of any of those comments.