


A senior medical professional has laid bare details of a “scary” staffing “crisis” at the hospital - and fears that recruitment issues are not only preventing rehabilitative care from returning to its previous level, but causing issues across the wider health service.
Facing a key vote this week on whether Samarès Ward should be reopened brought by Senator Steve Pallett, senior Health officials have in the past week released a promotional video and held briefings with politicians and the media to make the argument that Plemont Ward should remain the key rehabilitative facility.
Urging against placing too much weight on "emotive" accounts from individuals with experience of Samarès Ward, they instead argued that medics' voices needed to be heard on the matter.
Following those comments yesterday, two individuals contacted Express to share their experiences - an individual involved in rehabilitative care who worked on Samarès Ward and a senior nurse, whose account you can read HERE.
Due to the nature of their roles and concerns about repercussions from speaking out, Express has agreed to withhold the individuals' identities.

Pictured: Staffing was already starting to become an issue at the Overdale-based specialist rehabilitation facility when it was decided to close it.
Staffing was already starting to become an issue at the Overdale-based specialist rehabilitation facility when senior managers took the decision to close it in spring 2020, with little to no warning for staff working there.
At the time, the Government said that this was because the intention was to use it for covid patients and that it was not a cost-cutting measure - a position it has maintained despite challenges from politicians, islanders and other Health staff.
"What they're not telling anyone is the real reason Samarès closed is 1) it saved them a shedload of money, and 2) they couldn't staff it," a senior medic with significant experience of rehabilitation told Express.
"They are shedding and losing staff at phenomenal rates and these staff cannot be replaced - the people left are running harder and harder and going off with stress-related illness and leaving themselves.
"I believe it saved them over a million a year.
"The other reason is that they split the entire team that were Samares Ward and used them to plug gaps through the hospital through covid times. We didn't have the rehab unit then - it was broken up in order to plug gaps in the General Hospital. Rehabilitation nurses moved into acute wards to deal with acute patients - even though they are completely different skillsets.
"With pressure, we got a part of Plemont Ward and managed to pull back staff had left from Samarès Ward into there but still isn't the original team that we had."

Pictured: "They split the entire team that were Samares Ward and used them to plug gaps through the hospital through covid times."
Not only is the rehabilitation workforce now depleted, but the level of care being offered in the hospital is worse, the medic argues.
They explained that some patients on Samarès Ward - which cared for individuals recovering from strokes, head and body injuries among other conditions - spent more than a year there. The "lighter", more "open" environment was crucial for their recovery, they said.
"Samarès was sold as 'the' place to go to get better. It was off-site. There was a different culture, different environment. It looked out over the whole of St. Helier, the views were amazing."
Aside from the views, the facility also benefited from "wide open corridors, it had multiple areas and day rooms where patients could meet with their families and friends outside of their own rooms, every room was individual," the medic recalled.
"There were huge gyms there and rehabilitation areas, there was a kitchen where the occupational therapists could go through kitchen things, as well as occupational therapy rooms."
Crucially, patients were also able to go around the surrounding grounds in wheelchairs or zimmer frames with families and/or staff, and their loved ones also had the option of booking a wheelchair van to go out for the day.
But "there's nowhere to do that now", according to the medic.
"If you're on Plemont Ward and want to go outside, you firstly have to find staff free to take you - that's very unlikely. Then you're sat outside the casualty department on the pavement supervised by a member of staff or someone. Even simple things like a breath of fresh air is difficult."
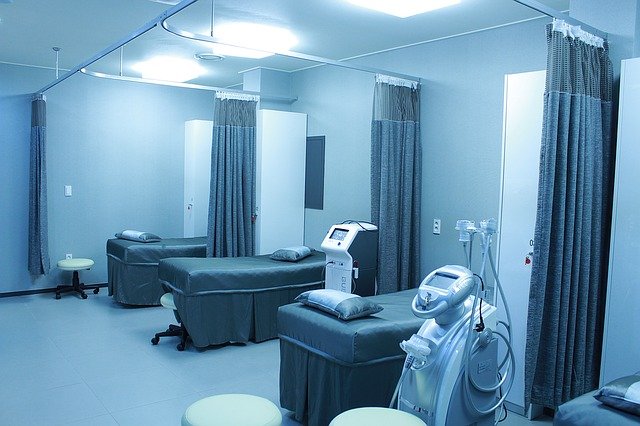
Pictured: Unlike Samarès, patients do not have individual rooms.
They went on to explain that, unlike Samarès, patients do not have individual rooms. Instead, they are on a "shared bay with at least five other people sharing a single toilet" - something that was not highlighted in the Government's video about care on the ward released last week.
"Think about the space people need to move around," the medic continued.
"When you think about the width of corridors when someone needs an enormous zimmer frame or people who need hoists, we don't have the space that's required and patients live in their bed or next to their bed. That's where they take their meals. A chair, a bed, that's where you do your socialising, that's where you live your life, and with only a curtain for privacy or dignity."
They added: "The environment matters hugely to patients in hospital and their rate of recovery and ability to leave. It's been proven multiple times - even the pictures on a wall make a difference. There are programmes and papers on landscapes and gardens because things as minor as that make a huge difference to recovery."
Yesterday, senior health staff admitted that the care being delivered currently at Plemont Ward needs improvements, but said that they had set up a 'Task and Finish Group' to work on bringing it up to standard.
The rehabilitation specialist told Express that this appeared to be a "knee jerk" reaction in the face of public pressure, having only held its first meeting shortly before Christmas. They added that, whatever improvements the group might make, it was a "nonsense" that the same level of care could ever be offered at Plemont Ward.
In the longer term, the Government plans to deliver more occupational therapy and rehabilitative care into the community. Yesterday, managers urged politicians not to make the "mistake" of supporting the reopening of Samarès and instead look forward to better care in future, when the Care Model is in place and the new hospital built.
But the rehabilitative expert Express spoke to decried this as a "waste" of resource, saying it would amount to paying qualified professionals to spend much of their day "driving around" to people, rather than making the most of their skills. This is something that more medical professionals would have raised, had they been properly consulted on the Care Model, they argued.

Pictured: The States Assembly is due to debate the reopening of Samarès today.
Even if politicians do support Senator Pallett's motion to return to providing a dedicated rehabilitation centre this week, the medic said they are not convinced that Samarès Ward could be properly staffed because of the crisis across the entire Health Department.
"We have new posts that we can't recruit to, and that's at all levels of medicine, nevermind therapy," they said.
They explained that many staff will start their shift in one area of the hospital, only to abruptly be pulled to support another short-staffed area where they are not familiar with the patients. Many individuals are working longer hours than they should be, and missing their breaks.
"We cannot recruit anybody... We are run on a skeleton staff supported by locums...It's frankly scary if you're a staff member, never mind a patient.
"...There is a veneer that we're all coping and nobody is. The problem is managers will never acknowledge that."
For some, the strain has manifested itself in stress-related sickness and early retirement. For others, it has resulted in "frustration" leading to poor behaviour among colleagues.
It was for that reason that Ministers' comments shortly before Christmas that there was "resilience" in the service were taken as a slap in the face by many in Health, according to the medic.
"That was the day we had four patients in casualty waiting on one bed in the hospital. There are times we've had three ambulances queuing on the ramp because there's no space in casualty... We certainly didn't have capacity and resilience is a nonsense when we constantly have doctors telling us, 'This is dangerous,' because we're giving them too many shifts.
"...Every time you see a colleague, they say, 'It's never been as bad as this, has it?'"
The solution, they said, lies in offering better salaries to attract new staff and perks like accommodation.
Decades ago, the medic recalled that salaries were around 30% higher than the UK, but now struggle to keep up with them given the high cost of living in Jersey.
No matter what happens in the Samarès vote, the medic says that the public and politicians must continue to keep pressure on the senior levels of the Health service.
With Plemont Ward, the medic said they feel it is the "nearest" Government has ever come to saying "we got things wrong".
"It took two years and enormous public pressure to even begin to think about it... I think we've started the ball rolling in terms of making the best of bad deal. That's two years too late. I think what politicians will have to do is keep the ball rolling to ensure what needs to be done happens. Otherwise next week, it will be forgotten."
Gov makes last-ditch attempt to win rehabilitation vote
OPEN LETTER: "Moving rehab services back to Overdale would be a mistake"
Stroke survivors and families make plea for Samarès Ward reopening
Government fights bid to reopen rehabilitation ward at Overdale
READER LETTER: Do not have a stroke in Jersey
Constable: Patients and hospital staff "let down" by leaders
Comments
Comments on this story express the views of the commentator only, not Bailiwick Publishing. We are unable to guarantee the accuracy of any of those comments.